The COMPLETE Guide to Understanding your Bloodwork
This article is a plain-English reference you can use to understand your bloodwork results. It goes into not just “good” or “bad” numbers, but why doctors are looking at these datapoints in the context of your overall wellness. If you’re interested in a particular result, search the name of the biomarker (ctrl+F on desktop or “Find in page” from a phone) to skip right to it.
There are three common blood tests; the CBC, the metabolic panel and the lipid panel. If you’re interested in only one of those tests, here are quick links that will scroll there for you:
Intro
For nearly all of human history, the body was essentially a black box. We ate and drank foods on one end, excreted them on the other, and somehow the body kept living and thriving. Everything “just worked” until one day an odd symptom would appear, and we’d have to wait and see if it was a passing ill-humour, or (gulp!) a disease that would cripple or kill us.
For the past 150 years, science has been finding new ways to peer into the body and understand what’s going on in there. We now have x-rays, MRIs, CAT scans, and ultrasound to get visual information from the inner body. But there’s no better way to know what’s going on at the cellular level than extracting a few tubes of blood and sending them to the lab.
When economists want to check on the fiscal health of a country, one of the first things they look to is the transportation sector. Shipping is how big interconnected economies work. If every plane, boat, and truck were to stop tomorrow, we’d be just a few days away from total societal collapse.
Blood serves the same function for the complicated, interconnected body. It takes about one minute for your blood to make a complete lap of your circulatory system, (much faster if your heart is pumping hard) and your body makes incredible use of each of those laps. As your blood circulates, it’s constantly picking up and dropping off nutrients, building materials, hormones, immune cells, and waste matter. It brings “just in time” shipping to the next level!
This is why a blood panel is such a useful diagnostic tool, and so often requested by your physician and health care providers. It’s the medical equivalent of lifting the lid on the black box and getting rich, detailed information on what’s going on inside. It’s magical!
Unfortunately, for the average person, the result of a blood panel is presented as the most unmagical, clerical chore you can imagine. A long list of obscure terms with even more obscure measurements next to them. Most of us simply look for numbers that are out of the range and chalk the rest up to medical esoterica.
If only you had a cool, smart friend to look at your blood test with you, and help you understand what all the terms mean, and why they’re important! Today we’re going to be that friend, and break down your blood test in simple, accessible terms. By the end of this article you’ll have a good working understanding of what a blood test tells you. Compared to someone from the 1800s, you’ll literally be a super-genius when it comes to the human body!
Let’s dive in. If you have a recent blood test handy pull it up and you can follow along. We’ll start with the most common blood panel, the Complete Blood Count (CBC).
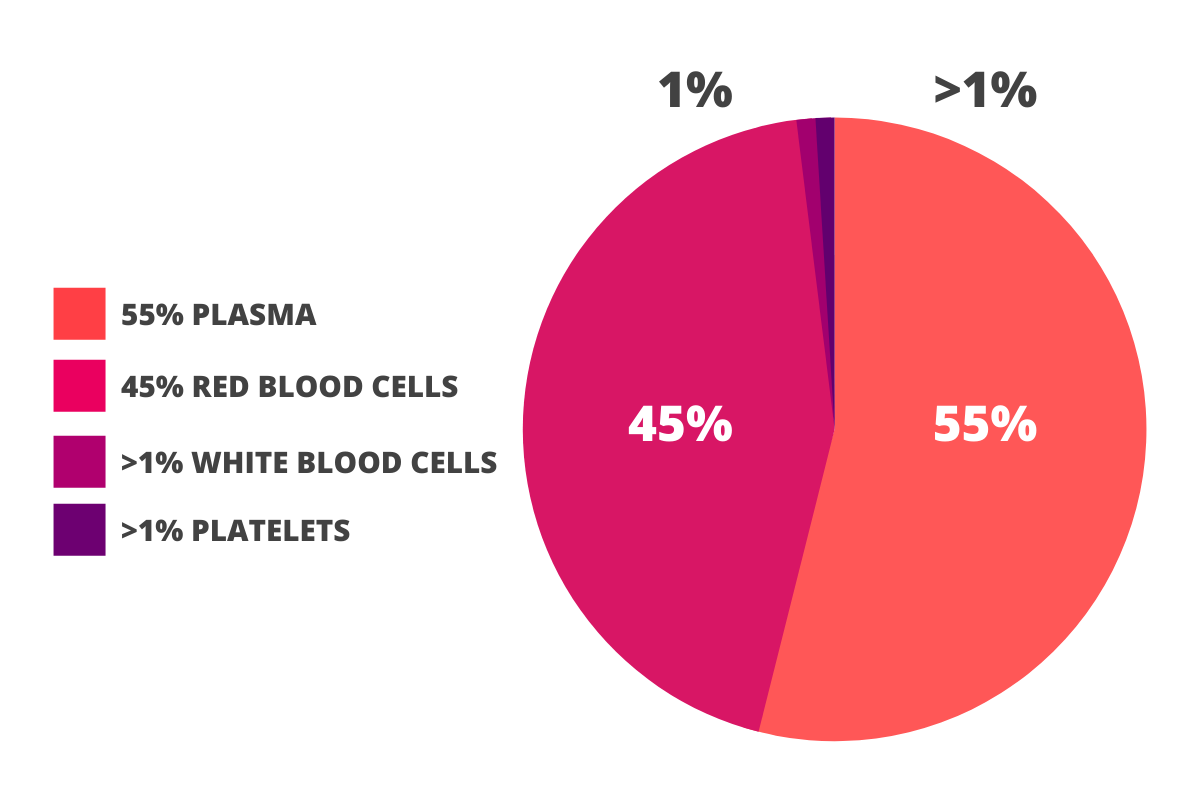
The most basic analysis that can be done on blood is simply looking at what kind of cells are present, and in what concentration. The main types of blood cells are red blood cells, which transport oxygen and carbon dioxide, white blood cells, which float around the body to fight disease, and platelets, which are little cell fragments that are able to form protective clots when part of the body is damaged. All of these structures are suspended in the plasma, a watery solution of salts and enzymes.
Most people don’t have a good sense of the ratios involved here. An average sample of blood will have the following breakdown:
This means to understand how many of the different cells you have, a lot of post-processing must be done on your blood sample. The sample is centrifuged, partitioned out, and sent through various machines. Making clever use of visual, electrical, and chemical analysis, the testing center can get highly accurate readings of how many of the different types of each cell you have.
In the old days, it was only possible to get a raw count of the cells, but with improved technology most blood tests now come back as a “CBC with Diff” meaning Complete Blood Count with Differential. This higher fidelity test can tease out not just the main cells but the smaller details of the bloodstream. Let’s go over what your CBC with Diff will have on it.
White Blood Cell Count
Your doctors are extremely interested in what’s up with your white blood cells, because they’re a leading indicator of the body dealing with disease and disorder.
If your WBC is low:
A low white blood cell count is a state called leukopenia and can indicate several problems:
It could point to bone marrow issues, since marrow is where white blood cells are made. This could be due to chemical exposure, either environmental (things like benzene and pesticides) or medical (things like chemotherapy and radiation). Certain viruses can also infect the bone marrow and reduce white blood cell count.
Autoimmune diseases like lupus, HIV, and rheumatoid arthritis will mistakenly attack white blood cells and lower their count.
Medications like antibiotics can destroy white blood cells.
The spleen is also a source of white blood cells, and infections or clots in the spleen will reduce white blood cell count.
If your WBC is high:
You might think more white blood cells is a good thing, but this too, indicates that the body is disordered.
If you’re actively fighting an infection, white blood cells will be elevated. This is a reason why doctors prefer that you don’t have bloodwork done while fighting the cold or flu — it throws off WBC.
Allergic reactions raise WBC.
Chronic stress will lead to higher white blood cell count.
Smoking is a constant irritant to the body and provokes higher white blood cells.
Obesity (and the chronic inflammation that comes with it) also causes high WBC.
Red Blood Cell Count
Red blood cells are little ovals filled with hemoglobin, a protein which is able to transport oxygen to the cells around your body, while picking up carbon dioxide waste on the return trip the lungs. The key molecule in hemoglobin is iron. Just as an iron nail is able to interact strongly with oxygen when it rusts, the iron in your red blood cells is able to dynamically interact with the O2 in your body, constantly picking oxygen up and letting it go when cells need it.
This is why your blood test will tell you not only your raw red blood cell count, but how much hemoglobin is present. You’ll also see a result called hematocrit, which shows what percent of your blood is red blood cells. Usually these metrics move together, but not always. For example, if you have a low RBC but normal hemoglobin, that indicates something is wrong with how the red blood cells are forming, as seen with such diseases as sickle cell anemia. If you have normal RBC and low hemoglobin, it points to a problem with your iron uptake, or lack of iron in your diet. But for most people, RBC, hemoglobin, and hematocrit will move in sympathy.
If your RBC is low:
Low red blood cell count is never good news. Your body is either not producing enough red blood cells, is destroying red blood cells at too high a rate, or you’re bleeding internally. Yikes!
Many diseases reduce RBC, most notably anemia, cancer, Hodgkins lymphoma, leukemia, and rheumatoid arthritis.
Problems in the bone marrow and kidneys will lower RBC, as both of these structures play a part in red blood cell production. The kidneys release a hormone which tells the bone marrow to crank of red blood cells.
Heavy menstruation can temporarily reduce RBC.
If your RBC is high:
Red blood cells are the energy transport of the body, but you don’t want to have too many of them! There are several root causes of a high red blood cell count:
Dehydration leads to high RBC, as the blood plasma is reduced, creating a higher concentration of red bloods cells per milliliter of blood.
The liver is responsible for so many things, but one of them is eliminating red blood cells that have reached the end of their useful lifespan (about 120 days). If the liver is compromised, for example with fatty liver disease or diabetes, then red bloods cells won’t be cleared properly and a higher RBC will start popping up on tests.
Platelets
Platelets are, in a word, weird. They’re not full cells, but fragments of cells that look like little amoebas with tendrils stretching out in all directions. Platelets float around the blood, waiting to spring into action if you sustain an injury. When the body signals an area is damaged, platelets flood the zone, and with their tendrils clog up the wound so that you don’t bleed out. This was an extremely helpful adaptation for life, as in the wild we tend to spend a lot of time getting bruised, poked, bitten, and broken.
On your blood test, you’ll see a test for platelets, and sometimes something called MPV (mean platelet volume) which measures the size of the platelets.
Low platelet count:
If you’re low on platelets, you’re at risk for excessive bruising and bleeding. Some things can cause this:
Leukemia and other cancers which affect bone marrow.
Chemotherapy and radiation therapy.
Heavy drinking is especially hard on platelet production.
High platelet count:
High platelets are also bad news, because it makes you more likely to have unwanted blood clots which travel around the body and cause trouble when they get stuck in blood vessels.
The most common cause of high platelet count is an infection. When the body is under attack, it goes into overdrive in platelet production. In older people especially a bad infection can lead to blood clots which become major medical issues.
Any chronic condition that leads the body to be held in a state of inflammation will lead to higher platelet counts as your system is in a constant battle to patch up the damaged areas.
Anemia, the lack of red blood cells, paradoxically leads to higher platelet count. Low RBC and high platelets is a trademark indicator of iron deficiency.
Lightning Round!
Now that you have a grasp of the three types of blood cells, you can easily understand what the more granular metrics are on the complete blood count blood panel. We’ll run through them quickly here.
MCV
This is mean corpuscular volume of your red blood cells. In other words, how big your cells are. If your red blood cells are too large it means there’s an issue with your nutrition, or even a liver disease. Small red blood cell size is a symptom of anemia, but is also seen in lead poisoning.
MCH and MCHC
This is mean corpuscular hemoglobin and is a measure of the average amount of hemoglobin in the red blood cells. It’s closely related to the problems of outlined about in the MCV red blood cell sizes.
WHITE BLOOD CELLS (basophils, eosinophils, neutrophils, lymphocytes, and monocytes)
It turns out there’s not just one type of white blood cell, but five (or more, depending on how you split hairs). The different white bloods cells are similar in appearance, but have small structural differences which allow them to specialize at tackling a particular type of threat to the body. Peering into the blood to tease out all these different types of white blood cells is what puts the “Diff” in “Complete Blood Cell Count with Differential.”
Basophils are like the town guards. When they see injury or an invader they alert their big white cell brothers to come solve the problem. They’re responsible for the histamine response.
Eosinophils are really good at attacking parasites and cancer cells. They also pitch in during allergic responses.
Neutrophils are the most common white blood cell. Their speciality is taking apart bacteria and fungi. Day and night they keep you healthy despite all the wild stuff that makes it into your body as part of daily life.
Lymphocytes are like the scientists of the white blood cell. They analyze bacteria and viruses and produce antibodies which fight off the invaders. When you get your COVID vaccine it’s the lymphocytes which give you the antibodies to quickly eliminate the problem when real COVID enters the system.
Monocytes are a shape shifting cell that are a jack of all trades. They’re able to transform their structure to either repair damaged tissue, or take down a bacteria, fungi, or virus.
How does your doctor use this granular information? If one particular type of white blood cell is overrepresented in the blood panel, it’s a clue as to what’s causing problems. For example, if there are a large number of neutrophils, it’s a hint that your issue is bacterial in nature. Higher eosinophils would point to a parasite. Isn’t it amazing what your blood can tell you!?
IG% and IG#
This is your immunoglobulin count. Immunoglobulin is the “goop” of protein antibodies in the bloodstream. High IG indicates your body is busy fighting off a disease or illness. If they remain high for multiple blood tests it points to a chronic condition. If you’re immunoglobulin is low, it’s usually a genetic condition or side effect of immunosuppressant medication.
This covers what you’ll see on a typical CBC with Diff blood panel. This blood test is most useful for telling your doctor about any high priority, immediate threats to your health. It’s also where blood disorders and cancer will make themselves known. If you get back a CBC panel with all normal numbers, rest easy knowing that your body is functioning well and in no immediate danger.
This is just the tip of the iceberg however! There are two other tests you’ll have access to as part of normal blood work. These are the metabolic panel and lipid panel. Let’s take them on and keep learning!
The Metabolic Blood Panel
There’s more in your bloodstream than just red and white blood cells. Your blood is also the transportation system for thousands of different molecules which have their own unique tasks.
Think of a busy subway train in the morning. On that train, you’d see people with all kinds of professions: bankers, baristas, teachers, construction workers, and so on. When the train stopped, all the workers would spill out and go to their various jobs, but they all need to ride the same train. So it is with the bloodstream, where vitamins, minerals, sugars, proteins, and all kinds of specialized molecules float in the plasma, stopping at different stations around your body to perform their essential tasks.
When a physician wants to see what’s going on inside your body, they can take a blood sample and check how many of these different worker molecules are present. If there are too few or too many of a certain molecule, it’s a good clue about the nature of any underlying problems. The test to find these specialized molecules is the Comprehensive Metabolic Panel (CMP).
The results of the CMP are even more confusing than the CBC. It’s easy enough to understand what a red blood cell count is, but phosphorus? Bilirubin? These sound like the terms of a medieval apothecary diagnosing your humours, not a modern medical test. What does it all mean?
We’re going to walk you through the ins and outs of this confusing blood test in simple, clear language, and give you a sense of what doctors are looking for when your results come in. We’ll start with the star of the show, fasting glucose level.
Glucose (fasting reference interval)
How do you power a jet? You put in jet-fuel. How do you launch a rocket? You put in rocket-fuel. How do you power an oxygen-breathing plant or animal? You put in life-fuel. Glucose is life-fuel. Glucose is a chemical arrangement of carbon, hydrogen, and oxygen that packs a lot of energy into a stable package.
Glucose is a saccharide, just like sucrose (sugar) and fructose (plant sugar). All the “-oses” share a similar molecular blueprint, with carbon forming a long “spine” where hydrogen and oxygen can easily be pulled off. This is why glucose goes by the street name “blood sugar.”
When a plant or animal needs energy, cells open up and let glucose from the bloodstream enter the cell walls. The glucose is then broken apart (metabolized), releasing their stored energy that allows the cell to complete its functions.
In short, glucose is really important, and that’s why it’s the top line item on your CMP results.
After eating (especially something sweet), glucose levels are elevated in the blood for several hours. Your doctor doesn’t want to be wondering if high glucose is from an internal problem or a jelly donut, which is why you need to have the CMP taken after at least 8 hours of fasting. 8 hours ensures your blood glucose is at background levels and not spiked from a food input. Hence, the result you see is your fasting glucose level.
If you have low glucose
We all have passing moments when our blood sugar drops. This will make you feel lightheaded and lethargic, but the body can usually rally, with the liver pumping out stored glucose to rebalance your energy levels. However, if you’re consistently showing low glucose on blood tests (hypoglycemia), it’s usually for following reasons:
• Adverse reactions to medications are the most common reason for low blood glucose. For example, quinine, an anti-malarial medicine, can lead to low glucose levels. Many medicines have this side effect, especially if the kidneys aren’t clearing the medicine quickly enough.
• Starvation and malnourishment will lower also glucose levels, most often seen in the developed world in cases of anorexia.
• If the pancreas is producing too much insulin, your blood glucose will be too low. This is a rare disorder caused by tumors on the pancreas.
If you have high glucose
This is called hyperglycemia, and is a much more likely result than low glucose. High glucose is related to the global epidemic of diabetes.
Since glucose is so key to cellular metabolism, the body has evolved a suite of complementary hormones to regulate how much sugar is in your blood. The most important of these is insulin, which floats through your system, opening up cellular doors to allow glucose to enter the cells. In type 1 diabetes, the pancreas doesn’t produce enough insulin for genetic reasons. In type 2 diabetes, the body has been exposed to so much insulin (often due to a high sugar diet) that the cells have developed insulin resistance and won’t open properly. High blood glucose usually indicates that something is going wrong with normal insulin function.
By far the main cause of high glucose levels in people’s CMP is due insulin-related problems. The metabolic panel is extremely useful to catch pre-diabetes and early diabetes. In the early stages, the patient won’t have any symptoms, but the high glucose will illuminate what’s going on, and preventative steps can be taken. If diabetes can be headed off at the pass before medication is required, patient prognosis and quality of life rises significantly. This is why a doctor is very interested in your glucose levels.
Beyond diabetes, there are other causes for high glucose. These include the following:
• Polycystic ovary syndrome (PCOS) which interferes with insulin uptake (and is often a companion problem with diabetes).
• Chronic stress will make your background cortisol levels too high. Cortisol is an antagonist to insulin and reduces the effectiveness of the insulin response.
• Infections like pneumonia or a UTI can temporarily raise glucose.
• Even without full-blown diabetic insulin resistance, obesity and a sedentary lifestyle will result in higher glucose levels. When you consistently have too much sugar in your blood you’ll feel fatigued, lightheaded, and headachy. Healthy blood glucose is the cornerstone of feeling well.
But glucose is just the tip of the iceberg in terms of what the complete metabolic panel is looking at. Let’s move on to the wacky electron-loving elements that make up your electrolytes.
Electrolytes (sodium, potassium, chloride, bicarbonate, and calcium)
The standard CMP will usually list these together, because they’re all different salts, and all share a similar function in the body. Let’s talk about what that function is.
When you see a humanoid robot move an arm or lift a leg, you know that what’s happening is that an electrical impulse is traveling from the processor to the servo in the limb. You could open up the robot and trace that little wire from the motor all the way back to the motherboard.
Organic life doesn’t have the ability to run metal wires from the brain to the different body parts. It has the challenge of sending signals through a bunch of water filled tubes.
Wiggle your left big toe right now. Isn’t it amazing that your brain can get the message all the way to the other end of your body, even though it’s not connected by anything but soggy cells and nerves?
Electrolytes are what make signal transfer through water possible. When placed in water, these molecules dissolve into negative and positive charged ions. When there are enough of these ions, a signal can successfully pass through the liquid.
These positive and negative ions also maintain cell integrity, as osmosis ensures that whichever side of the cell has a positive charge is where water will flow. If you were to suddenly remove all the salts from your body, your cells would instantly burst apart or shrivel up as this balance would be destroyed. This is why your physician is interested in seeing how many electrolytes are in your blood. They’re very important!
If you have low electrolytes:
Low sodium, potassium, chloride or bicarbonate can be caused by a number of issues, some easy to solve, others very serious:
• If someone is drinking too much water, they can dilute their electrolyte balance. This is why you want to stay hydrated, but not be drinking water all day long as some fad diets will advise.
• An under-active thyroid will lower electrolyte levels.
• Problems with the kidneys or liver not processing fluids correctly, creating salt clogs that result in low electrolyte readings in the blood.
• Anything that interferes with the hormone vasopressin will affect electrolyte levels. Vasopressin regulates how much water is excreted by the kidneys. Many medicines can scramble vasopressin production, including antidepressants, diabetes medications, cholesterol medications, and recreational drugs like MDMA (ecstasy).
• Certain infections and cancers will also impact vasopressin.
• Finally, one of the symptoms of heart failure is low electrolytes, which can create a self-perpetuating problem as low electrolytes create arrhythmias and knock on effects that weaken the heart.
If you have high electrolytes:
The most common cause of high electrolytes is dehydration. This can happen either through not drinking enough fluids, or because diarrhea or vomiting has quickly reduced your water content. When there’s not enough water in your system, electrolytes will stop ionizing and electrical balance is thrown off.
When someone dies from thirst, it’s usually because their brain can no longer communicate with the heart, the heart stops pumping, oxygen stops moving, and the brain cells die. Dying from thirst isn’t a water problem, but an electrical problem!
A poor diet high in sodium and processed food will lead to elevated electrolyte levels. This stresses the liver and kidneys, which have to put in overtime to filter the salts and maintain correct ion balance. As the liver and kidneys are worn out, electrolyte levels will gradually creep up year by year. If your blood test shows a one-off high electrolyte reading, your doctor will probably chalk it up to chance. But if year after year electrolytes are rising, it’s an early clue that something’s up!
Proteins (albumin, bilirubin)
The next set of molecules that the CMP explores is two proteins floating around your bloodstream.
You might think of proteins as having to do with making muscle, but a protein is any amino acid structure which performs a function in your body. As an analogy, look around at your kitchen appliances. They’re all made of metal and plastic, but depending on how that metal and plastic is structured, it can cool food down (refrigerator), heat it up (microwave), chop it into pieces (blender), or combine foods together (mixer). Proteins work the same way. Using just 20 amino acid building blocks, 20,000 different protein structures have evolved for all the many small tasks that are required to keep you alive and functioning. Some of those proteins are found in the blood, and are an important clue to the state of your health and wellness.
The CMP has a method of chemical analysis to tease out how many proteins are in your blood, which is what gives you the total protein reading.
This total protein is further broken down into the two most important blood proteins, albumin and bilirubin.
Albumin is a key housekeeping protein. It circulates through your system and helps usher hormones, vitamins, medicine, fats, minerals and various other molecules to the right place at the right time. You can think of it was the delivery van of the blood. It also regulates osmotic pressure in the blood vessels, making sure that your arteries and veins don’t leak fluid into the rest of the body.
Bilirubin protein is what decommissions blood cells, especially red blood cells, that have come to the end of their life. It takes apart the cells, tidies up the area, and then hitches a ride with albumin to reach the kidneys and dump the waste. This is why albumin and bilirubin are closely linked in function, and show up together in your total protein results.
The byproduct of red blood cell cleanup is a yellowish substance. When your cells take a lot of damage in one spot (like getting punched hard in the arm), the bilirubin comes and takes away the damaged cells, leaving a brown yellow smudge behind which we know as a bruise. When bilirubin is overactive and decommissioning way too many red blood cells, the entire skin can turn yellow, which is what causes jaundice.
In general, if total proteins are low, it indicates a problem at the protein factory — the liver. If total proteins are high, it indicates a problem at the protein garbage dump — the kidneys. Any diseases which touch on these two organs will show up in out-of-range albumin and bilirubin levels.
As you can see, the CMP is able to infer a lot of information about the liver and kidneys. Now that you have a sense of this relationship, we can cover the final, most confusing elements of the CMP.
Kidney Function (BUN, Creatinine, and eGFR [CKD-EPI])
Imagine a city with no water treatment plant. When you turned on your faucet, you’d get a mixture of whatever had gone into the sewers that day: medical waste, chemicals, feces, etc… Pretty gross to think about right?
The kidneys are the water treatment plants of the body. They filter, break down, and recycle material day and night. Healthy kidney function is critical for well-being.
There are three particular blood components which tell your doctor how well your kidneys are doing in this essential work. On your blood test results these are very unhelpfully named with confusing acronyms.
Let’s break them down.
BUN (blood urea nitrogen)
Your body is constantly in the process of breaking down cellular structures and rebuilding new ones. Every day, about 1% of your cells are replaced in this way. One of the most common byproducts of cellular break down is the simple molecule ammonia.
Ammonia’s molecular structure leaves a big, juicy nitrogen atom sticking out into the bloodstream. As it travels around your body, this nitrogen attracts carbon, hydrogen and oxygen, resulting in a strongly bonded molecule called urea. The kidneys have evolved to be adept at capturing and filtering out urea, which leaves the body as urine. When your urine has a strong ammonia smell, it’s an indication that high amounts of urea have collected in your bladder and are now leaving the body. (Incidentally, the yellow color of urine is a byproduct of the yellowish bilirubin byproduct discussed above.)
The CMP measures the amount of urea-bound nitrogen in the blood, hence the name blood urea nitrogen (BUN).
If your BUN is high, it can indicate that the kidneys aren’t doing their job and letting urea pass through the body without filtration.
If someone is on a high protein diet this will also increase BUN, because the liver is breaking down so much animal protein that the kidneys can’t keep up with the ammonia being sloughed off from the liver breaking down the amino acids.
Creatinine
You’ve probably heard of the bodybuilding supplement creatine. This molecule is produced in the liver and plays a role in how much work a muscle can do before it fatigues. People wanting to make more muscle will take supplemental creatine to push harder during their workouts and break up more muscle tissue. This tissue will heal bigger and stronger so they can bulk up.
Creatinine is the leftover byproduct of creatine, and is sent into the bloodstream as you flex and move your muscles. It’s the waste product of muscular exertion.
The useful thing about creatinine is that it stays in the blood at a steady-state concentration. A healthy body will almost always have the same amount of creatinine in the blood (accounting for body size and sex). This makes it a great benchmark for how well the kidneys are functioning (much more so than BUN which can be affected by hydration and diet).
Understanding creatinine allows you to unlock what’s going on behind the next hellish acronym on the metabolic panel.
eGFR (CKD-EPI)
The eGFR stands for estimated Globular Filtration Rate. This takes the raw amount of creatinine and runs it through an equation based on your race and sex. Which equation you ask? Why, the equation produced by the Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI).
Essentially this gives your doctor a more usable number than raw creatine stats (taking into account genetic factors), and estimates how well your kidney is filtering waste, using the “standard candle” of blood creatinine.
You don’t want high BUN or creatinine levels in your blood. You DO want a high eGFR. That means your kidneys are filtering efficiently.
Causes of kidney malfunction and bad blood results are varied, but the most common are no surprise:
• Diabetes damages the small, delicate blood vessels of the kidney, as glucose-rich blood is having to be filtered at a much higher rate than normal. This wears out the kidneys quickly.
• High blood pressure also stresses these filters, causing a slow loss of kidney function year over year.
• Smoking and other hard drug use puts the kidneys under pressure to filter toxins at a level far beyond natural background toxicity.
The message is clear. Eat right, exercise, and don’t smoke. Your kidneys have enough to do without added stress!
This leads us to the final set of results on the CMP, which come from the other end of the kidney-liver relationship.
Liver Function (ALP, ALT, and AST)
Oh no! Another set of impenetrable acronyms! Fortunately these share similar functions and are relatively easy to understand. All three are enzymes the liver uses to break down food into useful building blocks for the body.
If you ask someone what the most important organs in the body are, they’ll usually mention the heavy-hitters, the heart, lungs, brain, or stomach. Everyone forgets the humble liver, but it’s one of the coolest, most underrated parts of your body.
Imagine if you went to a restaurant and ordered pasta, but instead of a completed dish, the waiter brought you a bag of flour, some raw eggs, and a cup of water. You’d say “Are you joking? I can’t do anything with this! It’s not edible!” Just having the raw materials of food isn’t enough, you need a kitchen to assemble and bake the ingredients into a palatable, digestible dish. This is what the liver does for you. It takes all the raw ingredients that you ate, strips them down into component molecules, recombines them into what your body needs, then ships them out to your organs, bones, and muscles. The kitchen staff that it uses is a ragtag group of enzymes which are specially evolved to take apart specific combinations of food.
The CMP looks for three of these enzymes in particular.
Alkaline phosphatase (ALP)
This is the enzyme which breaks phosphate-bearing proteins in your food.
Alanine transaminase (ALT) – this used to be called serum glutamic-pyruvic transaminase which is why you sometimes see SGPT in addition to ALT on your results.
ALT is the enzyme which strips down alanine-bearing molecules into amino acid building blocks.
Aspartate transaminase (AST) – again, this had the old name of serum glutamic-oxaloacetic transaminase which is sometimes listed as SGOT on your results.
AST is the enzyme which converts aspartate and other proteins into usable amino acids.
What does high ALP, ALT, or AST mean?
Your doctor doesn’t want to see high levels of these enzymes in your blood panel. If they do, it essentially means your liver structure is compromised somewhere, and “leaking” enzymes into the bloodstream. The different enzymes give your doctor clues about where the problem may be. For example, high ALT alone indicates problems with liver tissue, while high ALT in combination with high ALP points towards a clogged bile duct.
The list of illnesses which can damage the liver is long, but the most common sources are familiar to you.
• Diabetes rears its head again, as insulin resistance forces the liver to work far outside its preferred glucose range. This creates a lot of stress on the liver tissue, which leads to a downward spiral as a less healthy liver is able to produce less and less healthy building materials for the body to recover and rebuild with.
• Excess alcohol consumption greatly stresses the liver and leads to scarring (cirrhosis).
• Hepatitis A, B, and C are all infections which inflame and scar the liver, reducing normal function.
• A variety of cancers and genetic diseases are centered around the liver and reduce liver function.
Checking the blood for higher than expected levels of ALP, ALT, and AST is the first clue that something is amiss in the liver, long before more serious symptoms show themselves, which is why your doctor wants to see those stats on your metabolic panel!
Imagine a child’s connect-the-dots picture. If there are only a few dots on the page, it’s impossible to figure out what the image is. But the more dots you add, the clearer the picture becomes. The granular data of the comprehensive metabolic panel gives your physicians a lot of dots to work with. And of course, as the outlines of a problem begin to form, even more precise tests can be ordered.
As you can tell, the CMP will quickly throw up red flags if anything’s amiss with your blood sugar, liver, or kidney function, and is a key part of diagnosing diabetic issues.
The last set of dots that we need to cover is the lipid panel. Here we go!
The Lipid Panel
The CBC helps your doctor understand how your blood cells and immune health are doing. The Metabolic Panel helps your doctor check how well your liver, kidneys, and other organs of energy-management are holding up. The lipid panel tells your doctor the status of the infrastructure of the tunnels that blood travels through.
Unlike the other panels, your lipid panel results are quite straightforward to understand, if you know the basics of cholesterol. Let’s shore up those basics now!
A Series of Tubes
When we walk around the world, doing fancy stuff like using computers and dancing the tango, it’s easy to forget that underneath our skin we’re just a series of mechanical processes. Unlike a human-fabricated machine, our organic processes tend to be wet, slimy, pulsing, and gooey, but they still involve real molecules being moved around to do different things that keep the system intact.
Anytime you have an engineering problem where one thing has to get to another in a chaotic environment, the solution is clear — build a tube. It’s how subways work, it’s how the internet works, and it’s how your body works.
You have all kinds of tubes running through you, but the most well-known are the arteries that deliver life giving oxygen and nutrients to your cells. Cut off any part of your body from the arterial pipes, and in an hour or so the starved tissue will start to permanently die.
Fortunately, it’s very rare for your blood tubes to get clogged up all at once (although it can happen with blood clots). But over time, just like the pipes in your house’s plumbing, your arteries can start to accumulate detritus on the walls of the tube. This buildup can harden into plaques that narrow the diameter of the tube.
If you’ve ever dealt with old pipes in a home, you’ll have seen the junk that clogs them up isn’t uniformly spread across the pipes. There are choke points where a certain amount of water flow hits a particular angle or bend and over time builds up a layer of crusty grossness. The same is true of your body. People don’t tend to have clogged arteries of the arm or back for example, it’s usually the heart and the brain where the tubes are the most twisty and prone to buildup.
High traffic intersections like this are likely points of plaque buildup.
This is serious business. The leading cause of death worldwide is ischemic heart disease, and number two is stroke, both a byproduct of arteries becoming narrow or blocked. Together, these two problems account for 27% of global deaths. If you go out to dinner with three friends, statistically speaking, narrow, hardened arteries will be the thing that kills one of you.
And what is it that’s clogging up those arterial pipes? It’s billions of tiny droplets of protein and fat called cholesterol. This is why your doctor is so interested in seeing how much cholesterol is floating around your blood -— it’s directly related to your incidence of heart-attack and stroke.
We all know “cholesterol” as this scary, menacing thing in our lives, but believe it or not it wasn’t until the early 1980’s that medical science agreed that it was the lipoprotein cholesterol that was behind hardening of the arteries. And it wasn’t until the 90’s that there was mainstream acceptance of the idea that not all cholesterol was bad. We’re still in new territory here, and learning more every year.
The lipid blood test teases apart the different kinds of fat and cholesterol in your blood, and presents them to you in 6 clean metrics. Let’s work through them step by step.
Cholesterol, Total
This is the raw reading of the amount of cholesterol in the blood in milligrams per Deciliter. This is usually a number between 100-350. Anything over 240 is considered too high, and will lead to your doctor recommending diet, exercise, or prescription interventions, depending on your situation.
Back in the 80s you would have gotten this number, and this number only. But we’ve learned a lot about cholesterol since then, and now understand that there are two varieties of it that have different effects on your body. This is the now famous LDL and HDL cholesterol types.
Before we get into LDL and HDL, let’s talk about why your body has cholesterol in it at all.
Your body needs fats to survive and thrive. Most of the fats that your system uses are fatty acids (long chains of hydrocarbons). These acids will lock into formations of three, forming a triglyceride, which then floats around the body, or is stored in tissues for later use (this is why we get fat when we overeat). You can think of triglycerides as being a lot like a drop of olive oil on your plate. They’re just little droplets of oil, a very simple lipid, but can be used in all kinds of ways. For example:
You can burn triglycerides for energy when you don’t have any food in your system.
You can use them to carry proteins and nutrients to different parts of the body (fat-soluble vitamins like A, D, E and K).
You can use them to create fatty layers around organs, preserving your internal temperature and protecting the cells.
This is why, after total cholesterol, the next item on your lipid test results will be:
Triglycerides
This is the amount of triglyceride packets in milligrams per Deciliter. Your doctor wants to see that you have enough of these fats, but not too many, which would be a symptom of a poor diet or a disease like diabetes or hypothyroidism.
But sometimes your body needs a fat that’s more than simple oil droplets. It needs lipids that have more structure and chemical interactivity. This is where cholesterol comes in. If fatty acids are like drops of cooking oil, cholesterol is more like a wax. It gets this structure because it’s not a pure lipid but a ball of gummed up proteins and lipids, called a lipoprotein.
The anatomy of a lipoprotein. Triglycerides hang out in the center, while proteins and various chemical stages of cholesterol form the waxy ball. These different molecular structures are able to interact with the body’s receptors to use the cholesterol as needed, kind of like a Swiss-army knife with its many different attachments.
Your body can put lipoprotein cholesterol to use in a lot of ways.
It’s used in your body’s cell walls, and gives your cells just the right combination of resilient squishiness and structural hardiness.
Your liver breaks down cholesterol into bile, which is used to metabolize dietary fat into useful triglycerides.
Cholesterol is an important component for your body to make its own vitamin D.
Your body also use cholesterol as a building block for various hormones, including steroids and sex hormones.
In simple terms, you can think of cholesterol as kind of an “intelligent fat”, because the proteins it contains are able to take part in much more complicated and varied chemical interactions than boring old triglycerides. It’s also really important. If you had zero cholesterol, you’d soon be a pile of bones and goo as your cell walls disintegrated.
The factory of the liver builds these little balls of cholesterol and sends them out to the bloodstream to do their work. At first, these balls are more lipids than protein. You can imagine the material as being very soft and pliable, like warm, thin wax. They are low density lipoproteins (LDL).
The problem with these light, fluffy, LDL balls is that when there are too many of them they tend to start accumulating on your arterial walls, forming those plaques which become dangerous as the tubes narrow and restrict blood flow. This is why LDLs are called the “bad cholesterol” (even though they’re a very important part of health). If all these acronyms confuse you, you can remember the “L” in “LDL” can stand for “lousy”.
As LDLs move through your circulatory system, the body takes off triglycerides here and there, and more proteins are added. This results in a higher ratio of proteins to lipids. Proteins are much denser and heavier than lipids, so our little ball of wax is now hard and more rigid. It has become a high density lipoprotein (HDL).
This dense little HDL ball keeps circulating through your systems, and as it bounces along, it does something special. Its proteins are able to pick up and bind loose bits of cholesterol that have gotten stuck to arterial walls. The HDL ball loads up on waste cholesterol and makes its way back to the liver, where the extra cholesterol is dumped back into the factory to make a whole new round of LDL to distribute the next wave of cholesterol around the body.
This is why HDL is called the “good cholesterol”. It literally scrubs your arteries of LDL plaques and recycles them for future use. That is, if there’s enough of it, which is why your doctor wants to see high numbers of HDL in your blood. You can remember the “H” can stand for “helpful.”
This brings us to the next two items on your lipid blood panel, after total cholesterol and triglycerides:
HDL
This is the amount of “helpful” high density lipoprotein in millgrams per Deciliter. A number of 60 or above is good. Below that and your doctor will want you to improve your diet.
LDL
This is how much “lousy” low density lipoprotein is in your blood in milligrams per Decililter. Anything above 130 is borderline, and above 160 is worrisome to your doctor.
On your blood test, you might see that LDL is marked as LDL-D or LDL-C. LDL-D means “LDL direct” and means the test actually measured how much LDL was in your blood. LDL-C means “LDL calculated” and means that the LDL number was extrapolated from the other numbers in the report rather than being directly measured. Both methods are highly accurate, the only difference is the type of testing equipment your lab used.
Next, you’ll see this:
Chol/HDL Ratio
This is your total cholesterol divided by your HDL levels. For example, if your total cholesterol was 150 and your HDL was 50, this number would be 3.0 The higher this number, the more concerned your doctor will be, as you have too little of the helpful cholesterol as a ratio to your total.
Finally, you’ll see this on your results:
LDL/HDL Ratio
This is your LDL number divided by your HDL number. It’s a quick way for your doctor to assess how healthy your ratio of bad to good cholesterol is. The lower the number, the better.
And that’s it! The lipid test is a way for your physician to understand how much fat and cholesterol is in your blood, and what your ratio of good to bad cholesterol is. When someone is overweight, eating poorly, and not exercising, there will be higher triglycerides, higher LDL, and lower HDL. This tells your doctor that your body is probably in the process of forming arterial plaques and that an intervention is warranted.
A good doctor will always prefer that you treat high LDL cholesterol with nutrition and exercise, but since so many patients are unsuccessful in these efforts, they’ll often reach for a prescription solution, usually a statin, which reduces how much cholesterol the liver produces. In later stages of very high cholesterol more intense medicine can be employed, but has more side-effects.
If you want to avoid all that, keeping your cholesterol in check is straightforward.
Try to get 30 minutes of continuous exercise a day.
Eat a diet that’s low in saturated fats (reduce dairy, butter, lard, ghee, oils, and animal fats).
Increase fruit and vegetable intake to boost nutrients and fiber intake.
Choose whole grains.
Don’t drink too much.
Reduce body fat.
Don’t smoke. Smoking makes everything worse, including cholesterol.
You’d be surprised how much a fitness intervention can turn around a bad lipid panel result. We’ve seen it hundreds of times with Kenzai trainees. Better cholesterol numbers that put a smile on your doctor’s face are just a few months away!
This concludes our epic run-through of what all those obscure acronyms and numbers mean on your blood panel results. The blood test is a miraculous way to peer into the black box of human physiology, and pinpoint small, easily fixed problems today that would become big, hard-to-treat issues later on. Take advantage of this miracle of modern science and get your blood checked every few years until your mid-40s, and then yearly after that. It’s important!